Chronic Hepatitis C
Hepatitis C (HCV) is a viral infection that can severely damage the liver and can even cause death. It’s spread through blood containing the infection, especially via shared needles used to inject street drugs. It’s the number one blood-borne infection in the US and the primary cause of liver cancer. Approximately 2.4 million people in the United States have hepatitis, but many aren’t aware that they’re sick because they don’t have any symptoms. So, the US Preventive Services Task Force (USPSTF) recommends that adults from 19 to 79 get screened for hep C.
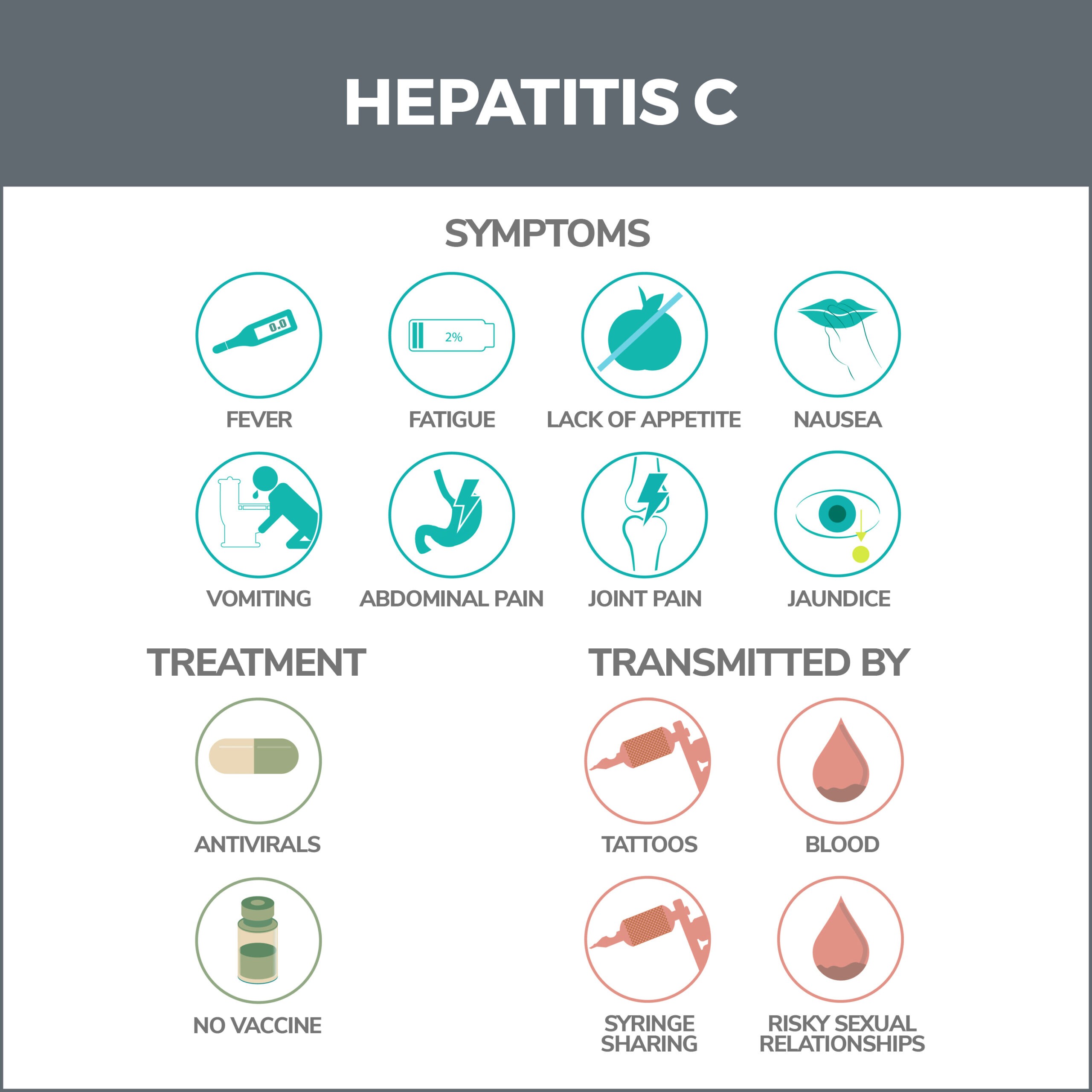
Types of Hepatitis C
There are two types of hepatitis C: Chronic and acute. Acute means a new, short-term infection, and chronic means a long-term infection.
Acute hepatitis C is a brief infection. It’s typically asymptomatic, meaning it doesn’t have noticeable symptoms. About 35% of people infected with acute HCV clear the virus on their own within half a year and without treatment. This is called spontaneous clearance. Experts are uncertain how or why the body does this.
As a precaution, your doctor may monitor you by giving you an HCV RNA test every four to eight weeks for half a year. This test indicates whether the hepatitis C virus is or isn’t in your bloodstream anymore.
You may still be susceptible to the virus even if you’ve cleared it or had successful treatment.
Chronic hepatitis C is a long-term infection when your body can’t fight it off. According to the Centers for Disease Control and Prevention (CDC), 85% of people with acute HCV will develop a chronic infection. It’s chronic if you’ve had it for six months or more. It can lead to liver fibrosis (the initial phase of liver scarring), cirrhosis (permanent liver scarring), liver cancer, liver failure, or death. Chronic hepatitis C is responsible for most liver transplants in the United States. There is no vaccine to prevent or cure the infection.
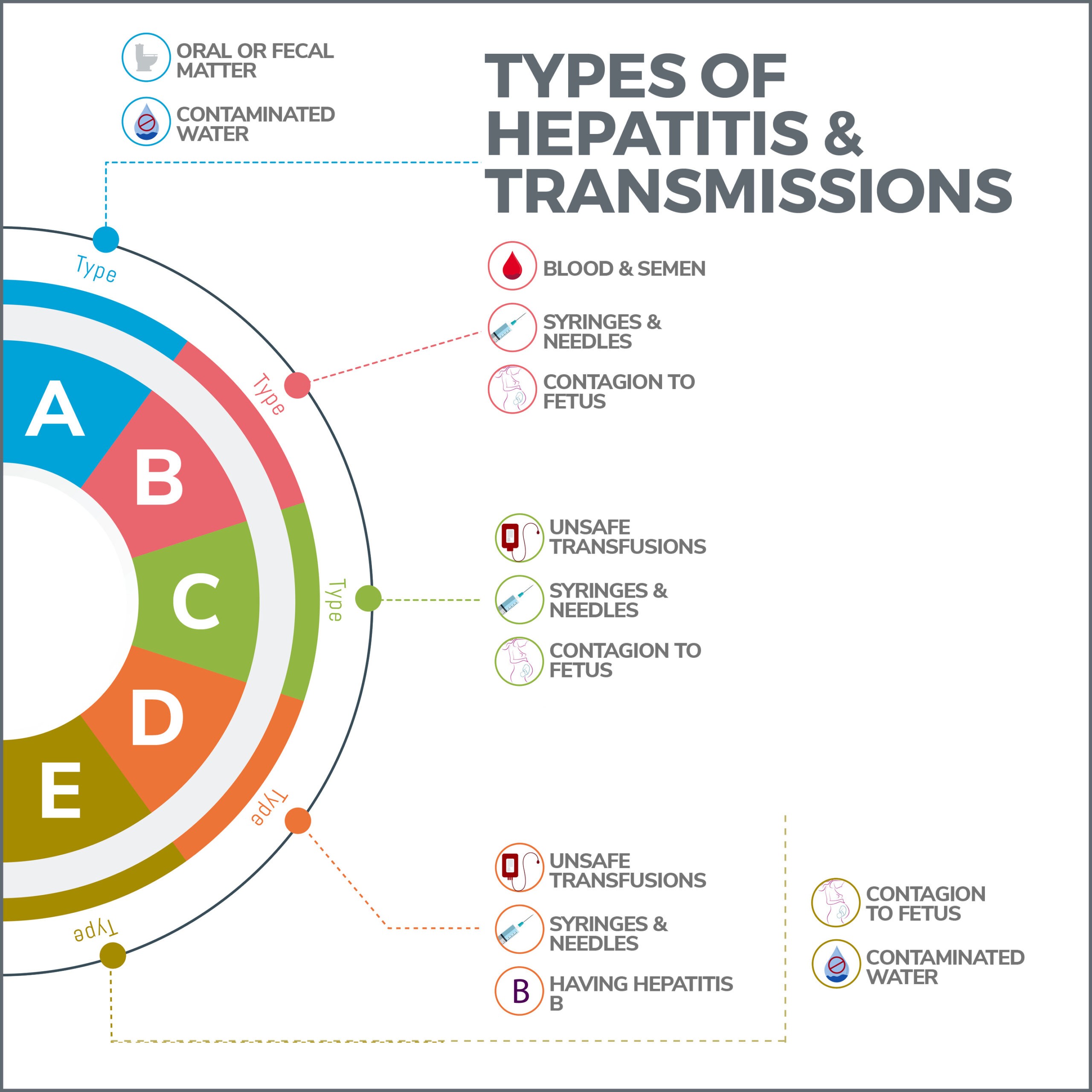
How Is Hepatitis C Spread?
Hepatitis C is primarily spread through blood-to-blood contact. Most people who become infected share unsterilized needles to inject recreational drugs such as heroin. It can also spread through shared drug paraphernalia, such as pipes to smoke methamphetamine or straws used to snort cocaine that may contain blood from mouths or noses. Other risk factors include:
- Getting a tattoo or body piercing with unsterilized equipment.
- Touching the blood or open sores of someone who is infected.
- Sharing personal items such as nail clippers, toothbrushes, or razors that may contain traces of blood.
- Accidental needle sticks in a healthcare setting.
- Being born to an infected mother.
- Long-term hemodialysis.
- Non-sterile medical equipment.
- Sex with an infected person. (This is a very uncommon way to contract hepatitis C.)
- Organ transplant or blood transfusion before 1992, when blood screening began.
- HIV diagnosis.
- Receiving clotting factor concentrates that were produced before 1987.
- Being a Baby Boomer – people who were born between 1945 to 1965. This age group is five times more susceptible to infection than other adults. Seventy-five percent of adults who have hepatitis C were born during these years. It’s unclear why this age group has a higher risk than others.
If you have any of these risk factors, it’s important to get screened.

Misconceptions About How Hepatitis C Is Spread
It’s a myth that you can get HCV through:
- Hugging.
- Kissing.
- Holding hands.
- Sneezing.
- Coughing.
- Food.
- Water.
- Sitting next to an infected person.
How Is Chronic Hepatitis C Treated?
Antiviral medications, also called direct-acting antiviral (DAA) pills, are typically administered to remove the virus from your bloodstream. Treatment is as simple as taking a pill. If the disease is caught early, these drugs have a 90 percent success rate.
Your doctor will choose the appropriate treatment depending on the extent of liver damage, previously used treatments, and the type of hepatitis C genotype you have. A genotype is the genetic makeup of different types of HCV, also called the strains of the infection. There are six genotypes, and each one reacts differently to different medications. Your doctor can select the most effective medication or combinations for you based on your genotype.
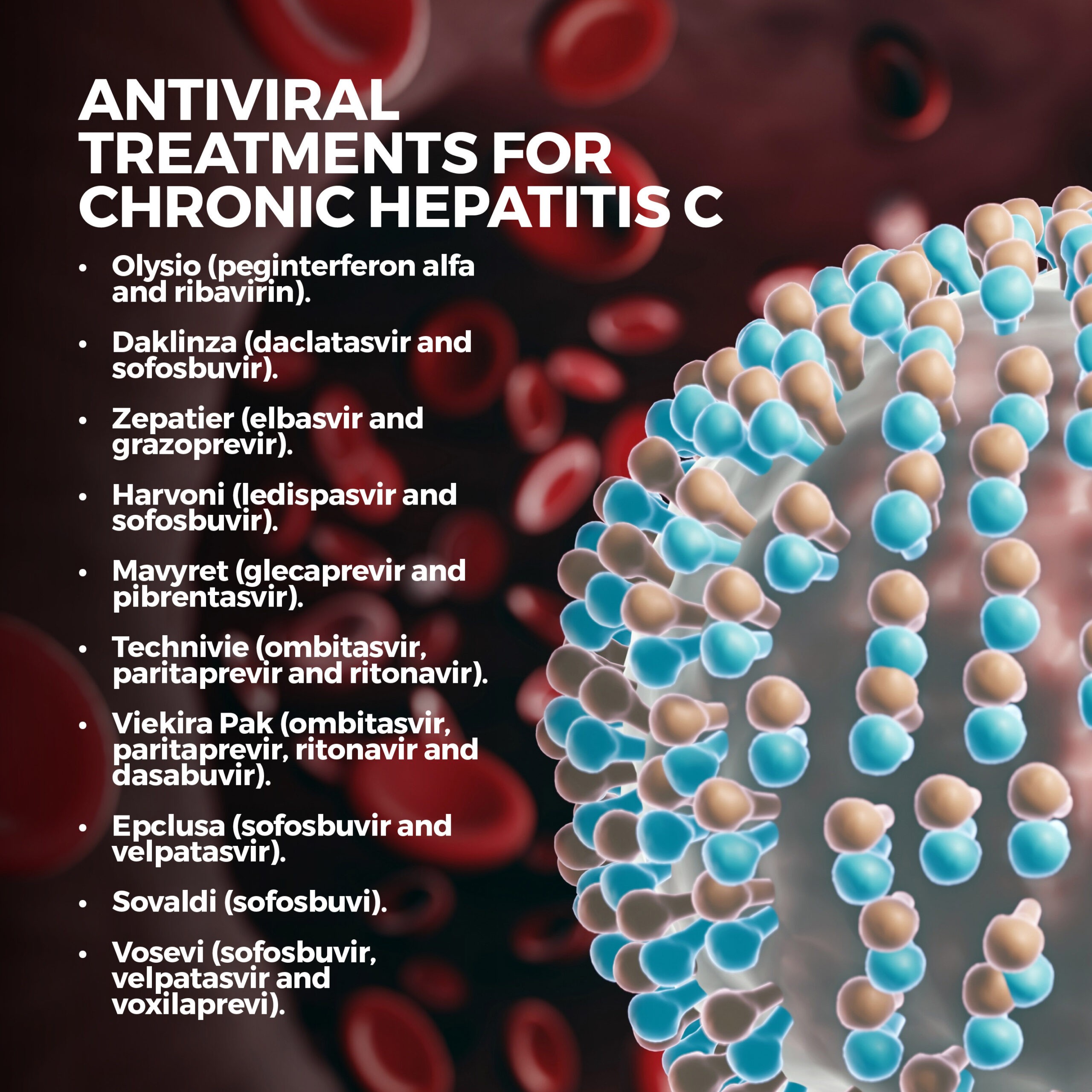
Antiviral treatments for chronic hepatitis C and their genotypes are:
- Olysio (peginterferon alfa and ribavirin) – genotype 1.
- Daklinza (daclatasvir and sofosbuvir) – genotypes 1 and 3.
- Zepatier (elbasvir and grazoprevir) – genotypes 1 and 4.
- Harvoni (ledispasvir and sofosbuvir) – genotypes 1, 4, 5, 6.
- Mavyret (glecaprevir and pibrentasvir) – genotypes 1, 2, 5, 6.
- Technivie (ombitasvir, paritaprevir and ritonavir) – genotype 4.
- Viekira Pak (ombitasvir, paritaprevir, ritonavir and dasabuvir) – genotypes 1a, 1b.
- Epclusa (sofosbuvir and velpatasvir) – all genotypes.
- Sovaldi (sofosbuvi) – all genotypes.
- Vosevi (sofosbuvir, velpatasvir, and voxilaprevi) – all genotypes.
You’ll take these drugs for eight to 12 weeks. During this period, your doctor will perform blood tests to determine the amount of HCV remaining in your bloodstream. If the virus is absent for at least 12 weeks after you finish treatment, the medication has effectively cleared the chronic hepatitis C, and you are considered cured.
If the first treatments are unsuccessful, your doctor may prescribe different medications that are more effective for your genotype.
How Do You Know If You Have Chronic HCV?
Chronic hepatitis C can be stealthy. Called a “silent” infection, it may be symptom-free and take decades to become evident. By then, liver damage may have become serious or irreversible. Or the disease may have symptoms that mimic less severe conditions, such as depression and fatigue.
Tests for Chronic Hepatitis C
Your doctor may order one or more of these tests to determine the extent of liver damage caused by chronic HCV:
- HCV antibody test (anti-HCV test) – Antibodies are disease-fighting proteins that are released into the bloodstream when you have an infection. If you’ve ever had hep C in the past or present, you’ll test positive for antibodies. If you test positive, you’ll have to get a hepatitis C RNA test.
- Hepatitis C RNA test – This test determines whether you currently have hepatitis C. It also shows how much of the virus is in your bloodstream (viral load).
- Liver biopsy – A liver biopsy is performed with ultrasound. A thin needle is inserted into the abdominal wall, and a small liver sample is removed for laboratory analysis.
- Transient elastography – Transient elastography is a non-invasive procedure that measures the speed of sound waves through the liver to determine its stiffness.
- Magnetic Resonance Elastography (MRE) – Magnetic resonance elastography is non-invasive imaging that uses low-frequency vibrations to measure the liver’s stiffness.
Liver Transplant
If you’ve had chronic HCV for many years, your liver could be irreparably scarred. In this case, you’ll need a liver transplant. During a transplant, your old, diseased liver will be replaced with a new, healthy one. This liver can come from someone who has died, although it may also be donated by someone who is alive.
Cancer and Chronic Hepatitis C
Chronic, untreated liver scarring can lead to liver cancer. Chronic hep C also raises the risk of non-Hodgkin’s lymphoma and neck and head cancers.
Cirrhosis can take more than two decades to develop. During that period, healthy liver cells are gradually replaced with scars. As these scars grow, your liver attempts to heal by producing new cells. Yet, the more cells your liver generates, the greater the chance they’ll mutate, causing malignant tumors.
Cirrhosis is associated with only about 20 percent of liver cancer in people with hepatitis C.
Contact Us
Don’t wonder if you have chronic hepatitis C. Whether or not you have symptoms; it’s important that you get the proper testing and care.
Contact us today! The team of professionals at GastroMD looks forward to working with you. We are one of the leading gastroenterology practices in Tampa Bay. We perform a host of diagnostic procedures using state-of-the-art equipment in a friendly, comfortable, and inviting atmosphere where patient care is always a top priority!




